FDA Approves Soliris to Treat
Generalized Myasthenia Gravis
Press Release: FDA Approves Soliris (Eculizumab) For The Treatment of Patients With Generalized Myasthenia Gravis (gMG)
Summary: Alexion Pharmaceuticals announced Sept. 23, 2017, that the U.S. Food and Drug Administration (FDA) has approved eculizumab (brand name Soliris) as a treatment for adult patients with generalized Myasthenia Gravis (gMG) who are anti-acetylcholine receptor antibody-positive. Soliris is the first in a new class of drugs to be approved for MG in the U.S.
Soliris is not a cure for MG, but it may lessen the symptoms experienced by people living with generalized MG. Soliris was tested in clinical trials in patients who had previously failed immunosuppressive treatment and continued to suffer from significant unresolved disease symptoms such as difficulties seeing, walking, talking, swallowing and breathing. Patients taking Soliris had improved scores on scales designed to assess quality of life and symptom burden including double vision, ptosis (drooping of the eyelids), swallowing, speech, breathing, and use of arms and legs.
Statement from MDA President and Chief Executive Officer Lynn O’Connor Vos:
“MDA celebrates the approval of Soliris to treat generalized myasthenia gravis — the first in a new class of drugs to be approved for MG in the U.S. — and we offer our deepest thanks to the dedicated researchers, and the individuals and families who participated in clinical trials to make this development possible.
“This is truly an unprecedented time, when more experimental therapies than ever before are reaching late-stage development and moving through the regulatory review process. In just the past few years, our community has seen six FDA approvals for drugs to treat neuromuscular diseases in MDA’s program — including periodic paralysis, Duchenne muscular dystrophy, ALS, spinal muscular atrophy and now myasthenia gravis. The origins of four of those six drugs can be traced directly to MDA research dollars.
“We are closing in on solutions for people living with neuromuscular diseases and will continue to fund critical scientific research, facilitate clinical trial participation, and advocate for policies that enable safe and effective therapy options to be made available as quickly as possible.”
Background: Patients with generalized MG experience muscle weakness in the head, neck, trunk, limb and respiratory muscles. An estimated 10-15 percent do not respond to treatments that are typically helpful in other MG patients.
Profound weakness throughout the body often is accompanied by slurred speech, impaired swallowing and choking, double vision, upper and lower extremity weakness, disabling fatigue, shortness of breath due to respiratory muscle weakness, and episodes of respiratory failure. Patients with generalized MG may require hospitalization, often involving intensive care unit stays.
Soliris is a terminal complement inhibitor that targets a part of the immune system called the complement system, which is responsible for helping antibodies clear damaged cells and potentially toxic microbes that could cause infections. In MG, antibodies whose job it is to target these toxic pathogens, instead inappropriately recruit the complement system and target the space across which nerve fibers transmit signals to muscle fibers, called the neuromuscular junction (NMJ). In patients with anti-acetylcholine receptor antibody-positive MG, the body’s own immune system turns on itself to produce antibodies against the acetylcholine receptor, a receptor located on muscle cells at the NMJ, activating the complement system. Soliris is thought to work in MG by inhibiting the complement pathway to prevent destruction of the neuromuscular junction.
MDA has not been directly involved in the development of Soliris for MG, but we have invested in previous research investigating complement inhibition as a therapeutic strategy for MG. In addition, MDA currently is funding research focused on developing improved complement inhibitors. (Soliris is a complement inhibitor drug.)
COSMETIC SURGERY HYPE:
WHICH PROCEDURES ARE ZEROS NOT HEROES?
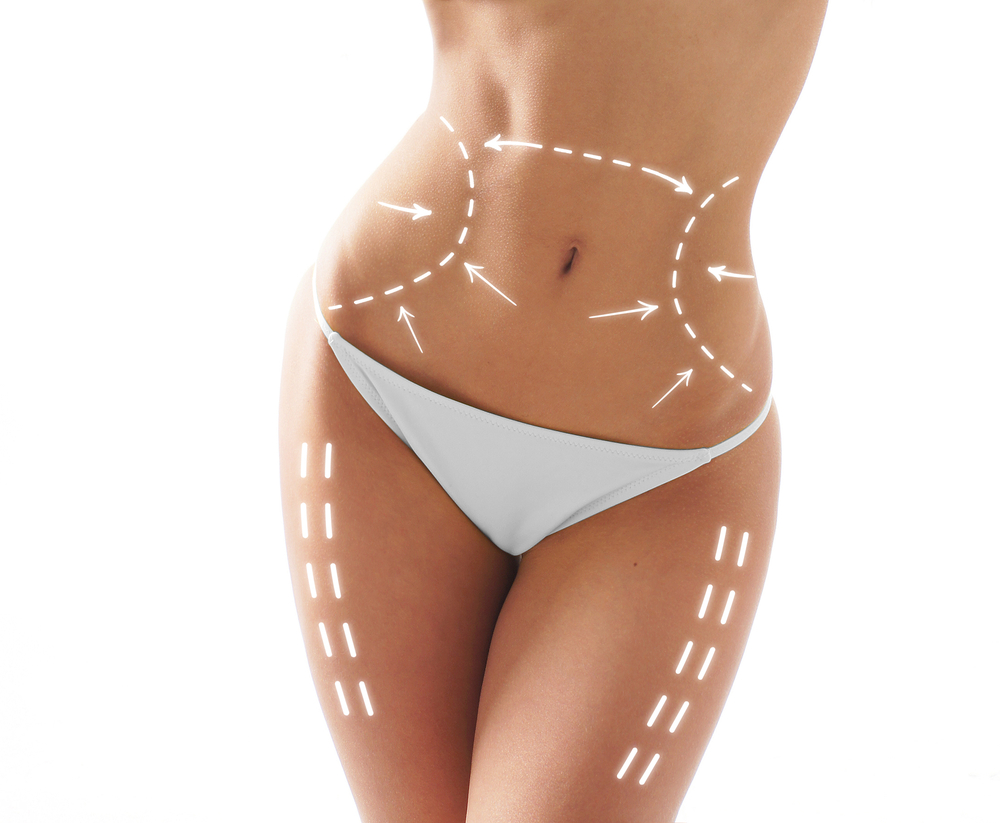
The name of the game today in cosmetic surgery is fast and non-invasive. The reasons are obvious. Nobody wants to be bedridden out of work and off the social grid as they recover. Fast results of a thinner, tighter, younger look within an hour is very alluring. How many of these seemingly miracle procedures actually do what they claim to? We turned to board certified Philadelphia plastic surgeon Dr. Kirk Brandow to breakdown cosmetic surgery hype; which procedures are zeros not heroes.
Kybella
This injection is made of deoxycholic acid, which is actually produced by the body naturally to absorb fat. The synthetic version is a fat cell destroyer injected into the pocket of fat below the chin. So far this is the only location on the body for which Kybella is FDA-approved. Dr. Brandow cautions, “Kybella may shrink fat but it’s also an acid which could burn the skin and cause an abscess or an open wound if placed too close to the skin. Equally important is that it can also destroy the deeper tissues as well which could lead to a dent just under the chin.” Another issue with Kybella according to Dr. Brandow is potential for ‘redistribution of fat’ to other areas of the neck when people gain weight, over time. “The loss of fat in this focused, Kybella, injected spot will look odd when areas around it are heavier looking.”
Instabreast
If you’ve ever considered a breast augmentation, it’s not hard to understand the appeal of “test-driving” a pair of implants for a day. This “try it before you buy it” procedure called Instabreast takes about twenty minutes in office. A saline solution is injected into the breasts until they are enlarged to the desired size. Surgeons who offer the procedure claim that it takes the guesswork out of planning an augmentation by providing patients with 24 hours of experience with larger breasts.
“This is crazy!!” says Dr. Brandow. “How do you anesthetize the breast before you shoot in the saline? Wouldn’t this hurt? Just the thought of it would scare off my patients. Additionally, implants on top of the muscle versus under the muscle look different and the size you use on top looks totally different from the one you would use under the muscle.” Dr. Brandow questions the safety of injecting saline under the muscle in office with a local anesthetic. “I would say it’s a recipe for a punctured lung! Additionally, I would love to know how a surgeon inflates a young, tight skinned, A- cup woman who wants a full C- cup, without causing a lot of pain during that injection.”
Mesotherapy and Lipodissolve as a Fat Dissolver
Several cosmetic surgeons and dermatologists agree that if there is one procedure to avoid when shopping for a slimmer look, it's one called lipodissolve, a shot that claims to dissolve away stubborn fat deposits. This shot is often part of “mesotherapy;” a shallow injection of a cocktail of substances using a fine needle. "There is really not a single scientific study to show that it definitely works," says Dr. Brandow. Are these chemicals safe when injected into fat? What happens to this fat? Where does it go? Dr. Brandow feels lipodissolve is an ill-advised treatment. “This is a non-FDA approved use of a material called lipostabil, which can dissolve fat and other structures however, it can cause pain, swelling, hard lumps, ulceration of the skin, and contour irregularities. None of the pharmaceuticals used for injection are FDA approved.”
Laser Liposuction
It seems like everything that has the word “laser” in it today is perceived as a state-of-the-art breakthrough, but in this case, using laser to assist in liposuction is not necessarily so. Laser liposuction uses lasers to liquefy the fat before it is removed, making it easier to vacuum out and they may also stimulate the production of collagen and elastin, which results in firmer, tighter, and smoother skin. Lasers may also coagulate small blood vessels in the area, which translates to less bruising. What’s the downside? Dr. Brandow points out that, “There is greater risk of burning and therefore, pain. Laser liposuction, Smartlipo and similar procedures add both time and money to the typical technique.”
About Dr. Kirk Brandow
Dr. Kirk Brandow is a board certified plastic surgeon with practices in the Philadelphia metro area. Named a “Top Doc” in Plastic Surgery by Philadelphia Magazine as well as nationally recognized for one of America’s “Best Plastic Surgeons” of this decade, Dr. Brandow is a trusted expert who has developed many innovative, minimally invasive procedures for the face, body and skin. These procedures include the Boomer Lift™, the 48 Hour Facelift™, the Scarless Breast Implant, the Multilayered Micro-Lipo Augmentation, the Tumescent Technique for Liposuction and the CO2 Laser Blepharoplasty.
He has been featured on local, national and international television programs including 20/20, CNN’s Headline News, Good Morning America, ABC Action News, TV Globo and Telemundo to provide updates and opinions on the latest trends in cosmetic surgery. Dr. Brandow where he has spoken out on the controversial issues of cosmetic surgery, advising viewers to take a more responsible and more realistic approach to the latest fads and gimmicks in Cosmetic Surgery.
Dr. Brandow served as an Associate Editor of the International Journal of Aesthetic and Restorative Surgery as well as a preceptor for many live surgical training conferences where he helped teach other doctors advanced techniques in Cosmetic Surgery.
Connect with Dr. Brandow via www.brandowclinic.com
KIND Snacks Urges FDA to Redefine “Healthy”

Company, with Support of Nutrition Experts Petitions U.S. Food and Drug Administration to Update Guidelines Established 20+ Years Ago
KIND Snacks, with support from leading nutrition, public health and public policy experts, has filed a Citizen Petition urging the U.S. Food & Drug Administration (FDA) to update its regulations around the term healthy when used as a nutrient content claim in food labeling. http://dnr.vnr1.com/2015/11/30/KIND_Snacks
KIND Founder and CEO Daniel Lubetzky explains that wholesome and nutrient-rich foods like almonds, salmon, olive oil and avocados cannot be labeled as healthy because of these foods inherent fat content.
The petition also reflects the importance of eating whole foods and foods made with wholesome and nutrient-rich ingredients as part of a healthy dietary pattern.
Currently, the FDA mandates that the word “healthy” only be used as a nutrient content claim to describe individual foods that contain 3 grams or less total fat and 1 gram or less of saturated fat per serving. Fish and meat must have 5g or less total fat and 3g or less saturated fat per serving to use healthy as a nutrition content claim.
The policy effort, which cites evidence from multiple nutrition studies and current federal Dietary Guidelines, is supported by a number of leading health and wellness experts including Dariush Mozaffarian, MD, DrPhD, Dean, Friedman School of Nutrition Science and Policy at Tufts; Sara Baer-Sinnott, President of Oldways; and Connie Diekman, Registered Dietitian and former President of the Academy of Nutrition and Dietetics.
For more information, visit KIND Snacks’ blog at www.KINDsnacks.com


